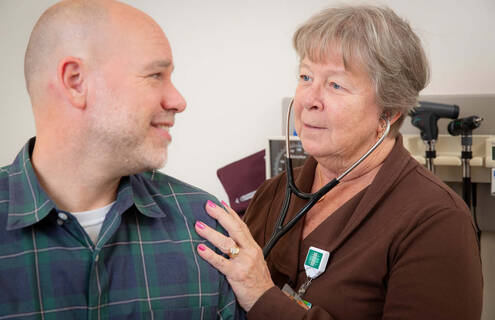
This gift allows us to prioritize the mental well-being of our staff, who are the key to delivering compassionate, patient-centered care at APD.
Susan Mooney, MD, MS, president and CEO of APDAlice Peck Day Memorial Hospital (APD), a member of Dartmouth Health has received a three-year grant from the Couch Family Foundation to implement the "Trauma Informed to Trauma Active" initiative, a groundbreaking employee mental healthcare program leveraging Eye Movement Desensitization and Reprocessing therapy. APD has partnered with Trivium Integrative Mental Health (Trivium) in Lebanon, NH, to offer employees access to this evidence-based intervention shown to treat post-traumatic stress disorder (PTSD), anxiety, and depression.
"This gift allows us to prioritize the mental well-being of our staff, who are the key to delivering compassionate, patient-centered care at APD," said Susan Mooney, MD, MS, president and CEO of APD. "By investing in mental health, we increase our workforce’s resiliency and strengthen our ability to consistently serve our community."
Among healthcare workers, nurses face disproportionately high rates of anxiety, depression, PTSD, and suicide, challenges exacerbated by the COVID-19 pandemic and incidents of verbal or physical assaults on healthcare workers. These factors impact not only their well-being but also the quality of care they deliver. These challenges extend to other healthcare workers as well.
“One of the benefits of this program is the immediate availability of access to mental health through our partnership with Trivium,” said Paula Seaman, MSN, DA, chief nursing officer at APD. “It can often take weeks to see a mental healthcare provider, but our employees can sometimes be seen the same day, and if not, within a few days. This new intervention follows a relatively short treatment course – anywhere from one to six sessions of 60 minutes each.”
Developed by Francine Shapiro, Ph.D., this therapy is extensively researched as a treatment for PTSD. A pilot program, launched in 2024 in partnership with Trivium, integrated this therapy, peer support, and onsite access to mental health clinicians for APD nurses. During the pilot, every participant reported decreased distress levels after intervention.
"In keeping with the Foundation’s principle of research informing practice, we are happy to support the continued implementation of this evidence-based trauma-informed model providing hospital employees access to critical mental health supports,” said Sara Vecchiotti, Executive Director, Couch Family Foundation. “Importantly, this project promotes the well-being of staff who play a frontline and pivotal role in supporting the health and resiliency of the greater community.”
In addition to the three-year expansion, the Foundation’s funding supports data collection and sharing insights with the broader Dartmouth Health community. Advanced assessment tools like the Posttraumatic Stress Disorder Checklist Scale will measure program effectiveness, while findings will inform similar initiatives across healthcare settings.
APD employees may access the program anonymously and free of charge for the first several sessions to treat PTSD that arises from events both in and outside the work setting. The hospital also works with Trivium to provide training to peer supporters to develop skills for their own self-care and wellbeing, emotional first-aid skills to help others, and the ability to recognize signs of acute stress.
About Dartmouth Health
Dartmouth Health, New Hampshire’s only academic health system and largest private employer, serves patients across New England. Dartmouth Health provides access to more than 2,300 providers in nearly every area of medicine, delivering care at its flagship hospital, Dartmouth Hitchcock Medical Center (DHMC) in Lebanon, NH. Its network of hospitals, outpatient centers, clinics and home care facilities, spans a broad geographical area. Year after year, DHMC is named the #1 hospital in New Hampshire by U.S. News & World Report, and is consistently recognized for high performance in numerous clinical specialties and procedures. Dartmouth Health includes Dartmouth Cancer Center, northern New England’s only National Cancer Institute-designated Comprehensive Cancer Centers and one of less than than 60 total nationally; Dartmouth Health Children’s, which includes the state’s only children’s hospital (Children’s Hospital at DHMC/CHaD) and more than 20 locations around the region; eight member hospitals in Lebanon, Keene, Claremont, Hampstead, and New London, NH, and Windsor and Bennington, VT; Dartmouth Health Home Care; Dartmouth Health Connected Care Center for Telehealth, serving patients as far away as Texas; and more than 30 primary and multi-specialty clinics across New Hampshire and Vermont. Through its partnership with Dartmouth College, Dartmouth’s Geisel School of Medicine and the White River Junction VA Medical Center, Dartmouth Health trains nearly 400 medical residents and fellows annually and performs cutting-edge research and clinical trials with international impact. Dartmouth Health and its more than 16,000 employees are committed to serving the healthcare needs of everyone in the communities it serves and to providing every patient with exceptional, state-of-the-art, personalized care. Learn more at dartmouth-health.org.